Some drugs can cause chemotherapy-related heart dysfunction
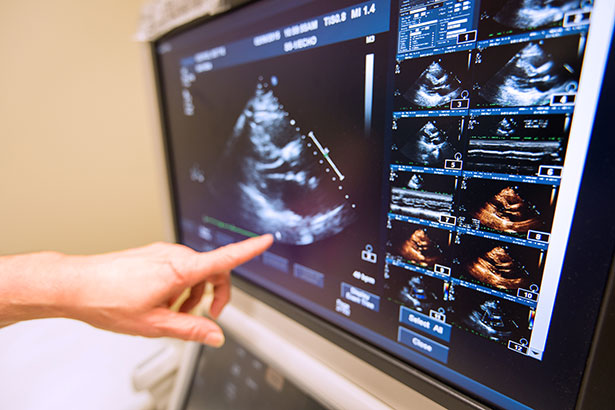
Expertise in cardio-oncology can be a decisive factor for patients challenged by the cardiotoxicity of cancer treatment who nonetheless need the therapeutic benefit of the medications.

Jay Erlebacher, MD, FACC, medical director, echocardiology laboratory at Englewood Hospital and Medical Center, has set up a cardio-oncology subsection in his lab and serves as the resident expert. “We have developed methodology to train our technical staff to do specialized heart function testing in patients who are getting chemotherapy, so we can follow their response to chemotherapeutic agents that are toxic to the heart,” he said.
Many cancer treatments can damage the heart, and patients with cardiac conditions treated with chemotherapy often have plans of care that differ from those who don’t. The top two cardiotoxic cancer drugs, doxorubicin (Adriamycin; others) and trastuzumab (Herceptin, Genentech), which typically are used in breast cancer patients, can cause chemotherapy-related cardiac dysfunction or weakening of the heart. Clinicians evaluate the heart function of patients receiving these drugs primarily by measuring left ventricular ejection fraction—the horsepower of the heart. A normal ejection fraction ranges from 55% to 65%, according to Dr. Erlebacher.
“The definition of chemotherapy-related heart dysfunction is when the ejection fraction drops by more than 10% and the final ejection fraction is under 50%. This happens in an unpredictable way in patients receiving Adriamycin and Herceptin,” Dr. Erlebacher said. “It is more common in people who have a history of heart attacks, valvular heart disease or other kinds of cardiomyopathy, as well as individuals with hypertension or diabetes, but this heart dysfunction can happen to young, healthy people, too. If clinicians keep pushing these drugs in someone whose heart has already become weak, they almost guarantee their heart function will be impaired and it can lead to congestive heart failure.”
Women treated for breast cancer with chemotherapeutic agents are at increased risk for developing congestive heart failure over the following five years, according to Dr. Erlebacher. Most doxorubicin toxicity occurs within six months of completing therapy and is dose-related, which is why patients taking doxorubicin receive an echocardiogram at baseline, at the end of chemotherapy, and then again six months later. Trastuzumab toxicity is not dose-related and can occur at any time, and thus, patients on this HER2-targeted therapy are evaluated every three months with an echocardiogram. Whereas damage from doxorubicin is often permanent, much of the damage from trastuzumab is reversible by holding or stopping use.
All cancer patients receiving potentially cardiotoxic drugs at Englewood Hospital are seen in the special subsection of the echo lab, which uses echo machines and employs two highly trained technicians to ensure consistent results. In addition to doxorubicin and trastuzumab, other drugs used routinely in oncology cause other problems, including clotting, atherosclerosis and severe hypertension. Tyrosine kinase inhibitors have adverse effects in a small percentage of patients and some new immunotherapies have been linked to rare lethal arrhythmias and reduced heart function.
Left Ventricular Global Longitudinal Strain
Recently, Englewood Hospital has started evaluating cancer patients for earlier signs of heart dysfunction using a newer measurement called left ventricular global longitudinal strain (GLS). GLS is assessed using automated speckle-tracking echocardiography to detect and quantify subtle disturbances in left ventricular systolic function. “The echocardiogram strain function looks at the relative motion of tiny speckles in the heart muscle,” Dr. Erlebacher explained. “In doing that, you can evaluate individual small segments of the heart in multiple planes.”
Alterations in GLS often precede any change in ejection fraction. If clinicians can detect subtle changes in heart function before they affect the overall ejection fraction, clinicians can provide standard treatments, such as ACE inhibitors or beta blockers, and reverse the course of many patients who would have developed heart dysfunction from chemotherapy. “The earlier you detect left ventricular dysfunction, the more successful you will be at reversing it,” Dr. Erlebacher said.
Dr. Erlebacher believes every center should have at least one or two cardiologists who are willing to take the time to specialize in cardio-oncology. “If you have a doctor who is not well versed and sees some of these changes, his first reaction may be to tell the oncologist to stop lifesaving chemotherapy,” he said. “The role of the cardio-oncologist is to watch the patient closely, treat if necessary, and permit the oncologist to give the patient as much chemotherapy as is safe, not stopping prematurely.” Thus, a trusting relationship between the cardiologist and oncologist is critical for the optimal care of cancer patients.
Posted September 2017
Some drugs can cause chemotherapy-related heart dysfunction
