Englewood Hospital has taken a leadership role in the use of insertable cardiac monitors
Long-term monitoring for atrial fibrillation with implantable cardiac monitors is a cutting-edge tactic for managing patients who have suffered a stroke, and it is an approach that neurologists and cardiologists at Englewood Hospital and Medical Center now regularly employ.

“We have been on the front line of advocating prolonged ambulatory electrocardiography [ECG] monitoring after stroke,” said Dennis Katechis, DO, a cardiologist at Englewood Hospital.
Patients admitted with an ischemic stroke are routinely placed on a heart monitor for the first 24 to 48 hours. In many cases, atrial fibrillation is difficult to detect within this short time period and the patient is discharged with a diagnosis of cryptogenic stroke (i.e., no cause is identified). Approximately 20% of ischemic strokes are considered cardioembolic, and atrial fibrillation is by far the most common cause of cardioembolic strokes.
Englewood Hospital was one of the first community hospitals to start using implantable cardiac monitoring after two major trials— EMBRACE (N Engl J Med 2014;370:2467-2477) and CRYSTAL AF (N Engl J Med 2014;370:2478-2486)— showed that prolonged ambulatory ECG monitoring was superior to conventional outpatient follow-up for detecting atrial fibrillation.
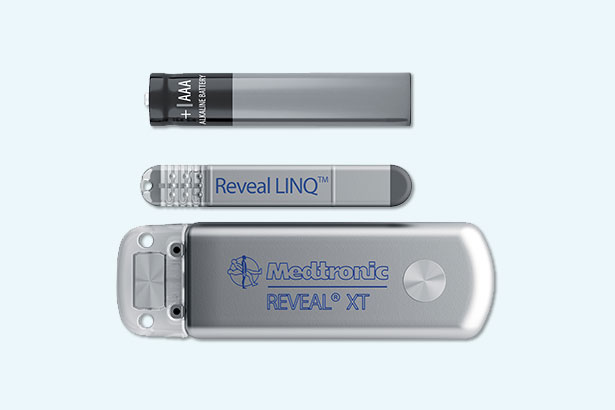
The EMBRACE trial demonstrated that atrial fibrillation was more readily identified in patients with cryptogenic stroke using an implantable cardiac monitor than with the conventional method of 24-hour Holter monitoring, specifically, 16.1% of patients at 30 days compared with 3.2%, respectively. In the CRYSTAL AF trial, an insertable cardiac monitor (Reveal XT, Medtronic) increased the rate of atrial fibrillation detection at six months from 1.4% to 8.9% for a control group that had received ECG monitoring.
Informed by these two studies, Englewood Hospital has taken a leadership role in the use of insertable cardiac monitors and has taken part in other trials involving implantable loop recorders.
Looped Recording
The latest monitoring technology, approved in March 2017, is the Reveal LINQ Insertable Cardiac Monitor with TruRhythm Detection (Medtronic), which enables physicians to continuously and wirelessly monitor a patient’s heartbeat for up to three years. The loop-recording device, smaller than a pen cap, can be inserted into subcutaneous tissue in the chest in a simple procedure that can be performed in an ambulatory setting. The device features a self-learning atrial fibrillation algorithm, which adapts to the patient’s heart rhythm over time. The cardiologist managing the patient is notified if a symptom is detected.

“The implant requires just a small incision and heals quickly,” said Lauren DeNiro, MD, medical director, stroke program at Englewood Hospital.
While many medical centers implant the device at a follow-up visit, Englewood Hospital does the procedure the day before a patient goes home from the hospital, so that no opportunity for early monitoring is missed. “A significant proportion of these patients—at least 15%— end up having atrial fibrillation,” Dr. DeNiro said. “This is important because it involves a different kind of treatment to prevent the next stroke. Prompt initiation of systemic anticoagulation is needed in most of these patients, as the presence of permanent or paroxysmal atrial fibrillation carries a cumulative risk of stroke that can be calculated based on a devised risk score.”
In addition to prolonged ECG monitoring, Englewood Hospital also has been on the forefront of nonpharmacologic therapy to prevent cardioembolic stroke. Grant Simons, MD, section chief, heart rhythm services, is responsible for the development and growth of the WATCHMAN program at Englewood Hospital.
The hospital participated in PROTECT AF, one of the trials that led to the approval of the WATCHMAN Left Atrial Appendage Closure Implant in 2015. This device, a self-expanding cage made of nitinol, provides an option for high-risk patients with nonvalvular atrial fibrillation who are seeking an alternative to warfarin or for those unable to take warfarin. Deploying the device in the left atrial appendage prevents a thrombus from forming and causing a stroke.
“The WATCHMAN device is truly revolutionary, a completely new standard of care in patients with atrial fibrillation to reduce their risk of stroke,” Dr. Katechis said. “It takes away the long-term risk of systemic anticoagulation for life.”
Posted September 2017
Englewood Hospital has taken a leadership role in the use of insertable cardiac monitors
