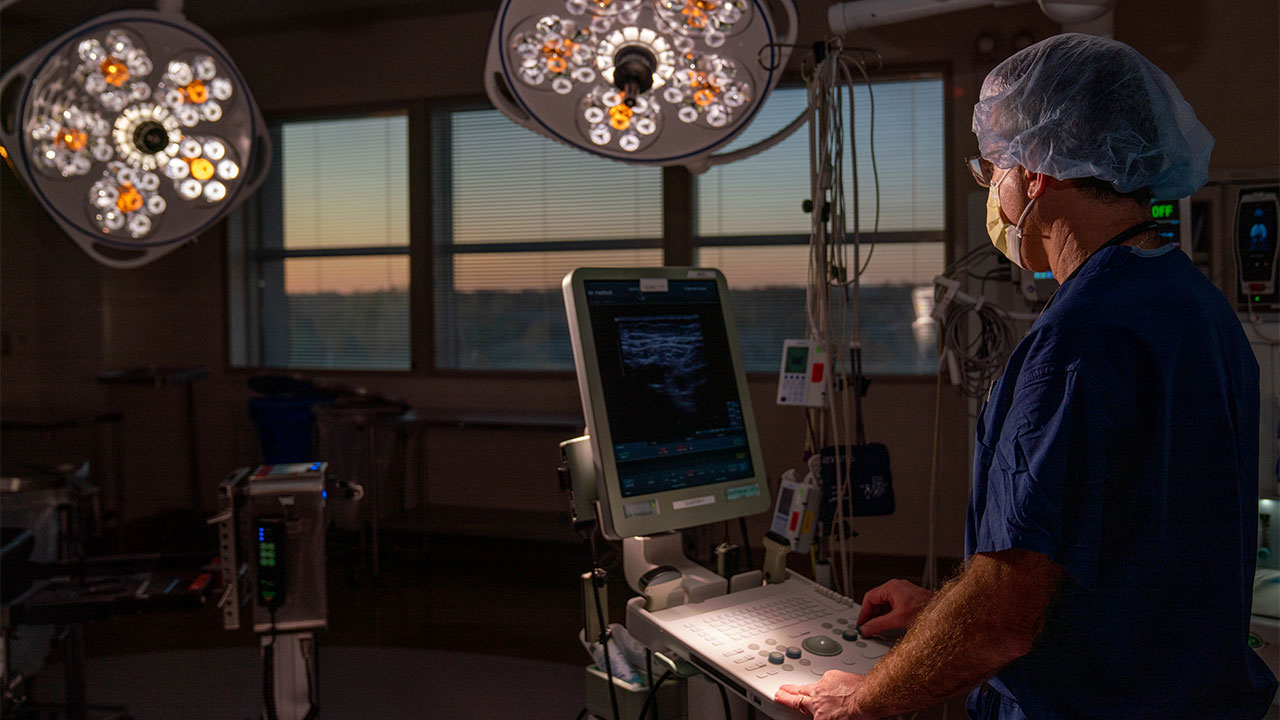
Anesthesiologists and pain medicine specialists are increasingly avoiding or reducing dosages in narcotics as the new standard of care. At the same time, advances in imaging and more portable ultrasound machines have allowed anesthesiologists to perform regional blocks of peripheral nerves with increased accuracy and frequency.
“Our precision with regional anesthesia has grown exponentially over the last few years as the imaging has become more fine-tuned thanks to the combination of ultrasound guidance and skill,” said Gregg Lobel, MD, the chief of anesthesiology at Englewood Health.
The ultrasound allows Dr. Lobel and his colleagues to visualize the nerve bundle that innervates the targeted area and to visualize the needle as it approaches the nerve. They stop the needle just short of the nerve to inject numbing local anesthetic. Ultrasound can visualize the local anesthetic surrounding the nerve.
The anesthesiology team can then thread a catheter through the needle to deliver a steady stream of site-specific nerve blocking agents to aid postoperative recovery for three days or more.
“By doing this, we reduce the need for opioids, which greatly reduces the future risk of substance abuse, so there’s tremendous upside to this method if you look at the risks and benefits,” Dr. Lobel said. “I’m glad to see it become the new standard of care.”
Opioids used for postoperative analgesia are frequently associated with adverse effects, including nausea and constipation, preventing smooth postoperative recovery.
“Suffering from those side effects causes stress,” Dr. Lobel said. “That’s not healthy for recovery.”
Regional anesthesia is commonly employed as brachial plexus blocks, paravertebral blocks, femoral nerve blocks, and sciatic and popliteal nerve blocks.
Academic research has found regional blocks to produce superior outcomes compared with IV opioids. A May 2020 study in the Journal of Bone and Joint Surgery (2020;102[10]:866-872) found that fascia iliaca nerve blocks following a hip fracture in a geriatric population were linked to shorter hospital stays, faster recovery and reduced opioid use. Similarly, on the other end of the spectrum, a review (Cochrane Database Syst Rev 2013;[12]:CD009587) found that a fascia iliaca compartment block for femur fractures in children provides better and longer-lasting pain relief with fewer adverse events than IV opioids.
Multimodal analgesia, which includes nerve blocks, is one of the most effective methods to reduce narcotic use in pain management, Dr. Lobel explained. It maximizes analgesic efficacy through the combination of several analgesic regimens, while minimizing undesired adverse effects, he said.
“We often turn to multimodal treatments since we can prescribe a combination of nonsteroidal anti-inflammatories with COX-2 inhibitors, acetaminophen and gabapentin, among others that work on different pain pathways,” Dr. Lobel said. “Each diminished pain pathway then decreases the need for stronger treatments, which helps us reach our goal of ultimately reducing the need for narcotics.”
A 2019 literature review published online by Orthopedic Surgery (2019;11[5]:755-761) found multiple benefits of multimodal analgesia for total knee arthroplasty when compared with standard care: greater pain relief, better knee recovery, and reductions in opioid consumption and related adverse effects. “In pain management at Englewood, we’re dedicated to working with the patient to deliver the best outcomes that accelerate recovery and decrease the need for opioids,” Dr. Lobel said.
As a specialist in pediatric anesthesiology, he finds that commitment strikes a chord with parents who are concerned that childhood sports injuries will introduce their kids to narcotic pain medicine. “They’re usually relieved to find that our multimodal approach with nonopioid analgesic medications and regional anesthesia mean their kids won’t take anything much stronger than Tylenol.”
Posted on December 17, 2020
