Suspect sleep—or the lack of it.

That is the recommendation that Kirk Levy, MD, gives physicians when a patient complains of a variety of symptoms that can seem unrelated to obvious daytime drowsiness. Patients may report heartburn, difficulty losing weight or morning headaches. They might mention depression and anxiety, or type 2 diabetes.
Couple these seemingly unrelated symptoms with fatigue, and the patient likely has sleep apnea. Although this is the most common sleep disorder, with more than 20 million sufferers in the United States, research has shown it is vastly underdiagnosed.

Dr. Levy and Mitchell Engler, MD, the comedical directors of the Center for Sleep Medicine at Englewood Health, are working to raise the profile of sleep apnea and other sleep disorders that can result in disruptive sleep cycles recurring hundreds of times each night. “The most common problem we encounter is that sleep apnea is not diagnosed because patients are not being asked the right questions,” Dr. Levy said.
To identify sleep apnea, physicians first need to ask their patients about their quality of sleep, along with accompanying breathing patterns (sidebar). If the diagnosis is suspected, polysomnography or another at-home sleep apnea test is performed. But without proper questioning, testing may not even be conducted.
Risk factors for sleep apnea include being overweight (body mass index of 25-29.9 kg/m2 ) and obese (body mass index of ≥30 kg/m2), although 50% of people with the condition are not obese. Also included is having a large neck circumference (men, ≥17 inches; women, ≥16 inches); having large tonsils or adenoids; other distinctive physical attributes including deviated septum, specific shape of head and neck, receding chin, enlarged tongue; nasal congestion or blockage caused by a cold, sinusitis, allergies, smoking, etc.; throat muscles and tongue that relax more than normal during sleep (possibly due to alcohol use, sedatives or advanced age); and a family history of sleep apnea, which may be the result of hereditary anatomic features or medical conditions that are genetically based.
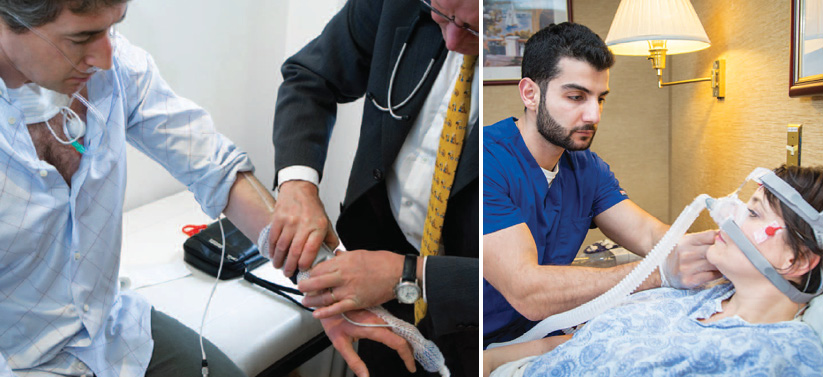
Generally, sleep apnea is treatable, according to Dr. Levy, by using a continuous positive airway pressure (or CPAP) mask over the nose. But left untreated, sleep apnea can result in serious health consequences over time—the symptoms mentioned above, and also mood change, memory loss, weight gain, risk for a cardiovascular event and impotence. Sleep apnea is even a major contributor to car accidents, as sleep-deprived drivers have up to a 15-fold greater risk for accidents. Drivers who have gone without sleep for 24 hours are equivalent to those who have a blood alcohol concentration of 0.10%, according to the CDC, which is higher than the nationwide limit of 0.08%.
“Doctors need to think about sleep apnea,” Dr. Levy said. “Most patients are not going to present with the complaints, so if you do not have it in your mind to screen for it, you’re not going to find it. Just understand it is frequent. It’s out there, and you need to keep it in the back of your mind with patients with these risk factors.”
To assist with the diagnosis and management of obstructive sleep apnea in adults, the American College of Physicians developed a clinical guideline (J Clin Sleep Med 2017;13[3]:479-504).
If patients answer yes to any of these items, they might have sleep apnea or another sleep disorder, and they should be referred to a sleep medicine specialist for evaluation:
- I snore every night.
- I experience daytime sleepiness.
- I wake up gasping for air.
- I wake up with heartburn/reflux.
- I have trouble losing weight.
- I have morning headaches.
- It is hard for me to stay awake while driving.
- I’ve been told that I fall asleep incredibly fast.
- I’ve been told that I stop breathing while I sleep.
Insomnia as a Comorbidity
Sleep apnea has been found to coexist with insomnia, with some statistics showing that one-third to half of people with sleep apnea suffer from sleeplessness (Sleep Med Rev 2017;33:28-38). To combat insomnia, physicians at Englewood Health’s Center for Sleep Medicine recommend strategies to promote better sleep, such as abstaining from alcohol around bedtime, as metabolizing alcohol overnight can cause wakefulness, thus fracturing sleep. They also recommend limiting screen time to reduce exposure to blue light; practicing relaxation exercises; and dedicating a bed to sleeping only, keeping reading a book or watching television to another room. “Another item to ban from the bedroom is the clock radio,” Dr. Engler said. Glancing back and forth to see how much time there still is to sleep, or to count how much time was wasted in sleeplessness, can “turn your brain into overdrive,” he said. Even with dedicated efforts, a switch to more regular sleep won’t happen overnight. “This is not easy to do. I tell my patients with insomnia: ‘You didn’t get this way overnight, and it doesn’t go away overnight. It takes work, but ultimately you’re retraining your brain to associate bed with sleep
Posted August 2019
